Abstract
Purpose: To describe the diagnosis and management of enterocele with high risk of bowel ischemia in patients with pelvic organ prolapse.
Methods: We describe the clinical case of an 81-year-old patient, hypertensive, obese, anticoagulated because of an atrial fibrillation and pelvic organ prolapse. Initially, conservative treatment was offered due to the high surgical risk, but sometime later the patient came to the emergency department with enterocele and risk of intestinal ischemia.
Results: After placing the patient in the Trendelenburg position and applying ice to the perineum, the prolapse is reduced. Subsequently, urgent surgical intervention is performed with a total vaginal hysterectomy, anterior colporrhaphy, Ritcher's operation and colpoperineorrhaphy. This intervention solved the patient's clinical condition and also avoided the small bowel ischemia.
Conclusion: The diagnosis of advanced enterocele with risk of intestinal obstruction is a very rare but potentially serious clinical case. The immediate recognition and management are very important because of the risk of vaginal rupture, intestinal necrosis, and also systemic infection.
Keywords
Prolapse, Enterocele, Intestinal obstruction, Surgery
Introduction
Pelvic organ prolapse (POP) is an entity produced by the descent of one or more organs from their usual anatomical position: uterus, vagina, urethra, bladder, rectum, sigmoid colon, or small bowel [1]. It is a common condition, and the prevalence increases with age [2] as a consequence of the failure of the supporting structures, accounting for up to 30% of major benign gynecological surgery in our environment [1]. It is a complex and multifactorial pathology in whose care three medical-surgical disciplines are involved, because urinary, genital, and rectal functions may be compromised [3].
Enterocele is a hernia of the small bowel into the vagina [4], because the peritoneal sac containing small bowel or omentum extends into the rectovaginal space that separates the vagina from the rectum [2]. They can be classified according to etiology, with traction enteroceles usually found in association with another anterior, middle, or posterior compartment prolapse [2]. Most cases published in the literature describe enterocele associated with vaginal vault prolapse after hysterectomy [5,6]. Clinically, patients usually report a sensation of pelvic lump or pressure, and sometimes pain or bleeding due to ulceration of the prolapsed organ if it extends beyond the introitus [2]. In addition to genital symptoms, they may also present urinary symptoms such as incontinence, urgency, dysuria, tenesmus, frequency of urination, or digestive symptoms with difficulty in emptying the rectum or obstructive defecation [3].
The management of these patients aims to reduce prolapse in order to improve their quality of life [2]. Pessary as first-line treatment in these cases is unsuccessful, because the pushing of the bowel contents leads to expulsion of it. As for the rest of POP, treatment, both conservative and surgical, would only be indicated in symptomatic cases or those with associated conditions [3,7]. Surgical repair of enterocele represents a challenge for pelvic floor surgeons, and should include removal of the hernia sac with correction of the fascial defect, approximating the pubocervical and rectovaginal fascia to close the hernial port [8]. Urgent intervention is rarely required, but in cases where the enterocele is associated with small bowel obstruction and cannot be reduced, emergency surgical treatment would be indicated to try to avoid intestinal necrosis and systemic infection [2].
We present the case of a patient with an advanced enterocele requiring urgent surgical repair due to the associated risk of intestinal complications.
Case Report
An 81-year-old patient, hypertensive, obese, anticoagulated with Rivaroxaban for atrial fibrillation, with a history of laparoscopic right hemicolectomy for adenocarcinoma of the rectum in 2018. Her gynecological and obstetric history included 4 euthecological deliveries, none of which were macrosomic, and menopause at the age of 60. Follow-up was done in the pelvic floor unit for pelvic organ prolapse and mixed urinary incontinence. Examination revealed total pelvic organ prolapse, with eversion of the vagina, grade IV enterocele according to the Baden-Walker classification [9], introitus amplitude greater than 2.5 cm and decreased vulvo-anal distance. The cough test was negative even when the prolapse was reduced. The 2D vaginal ultrasound showed a retroverted uterus with linear endometrium and atrophic ovaries, and integrity of both anal sphincters. Initially, conservative management was considered due to the patient's comorbidity, and after reduction of the POP, a number 80 pessary was inserted associated with closure of the perineum with three loose stitches of resorbable material under local anesthesia in the consulting room [10].
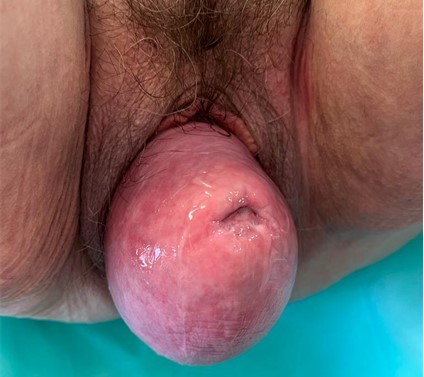
At the next examination, pessary expulsion and recurrence of total pelvic organ prolapse was observed, with intestinal loops included in the peritoneal sac, and total eversion of the vagina (Figure 1). Surgical intervention was proposed, but it was rejected due to an unfavorable preoperative risk score – ASA Physical Status Classification System – [11] ASA III, so a pessary was placed again with stitches in the perineum, while a cardiological assessment was requested on the recommendation of the Anesthesia Service.
Figure1: Total pelvic organ prolapse with vaginal eversion and grade IV enterocele [9].
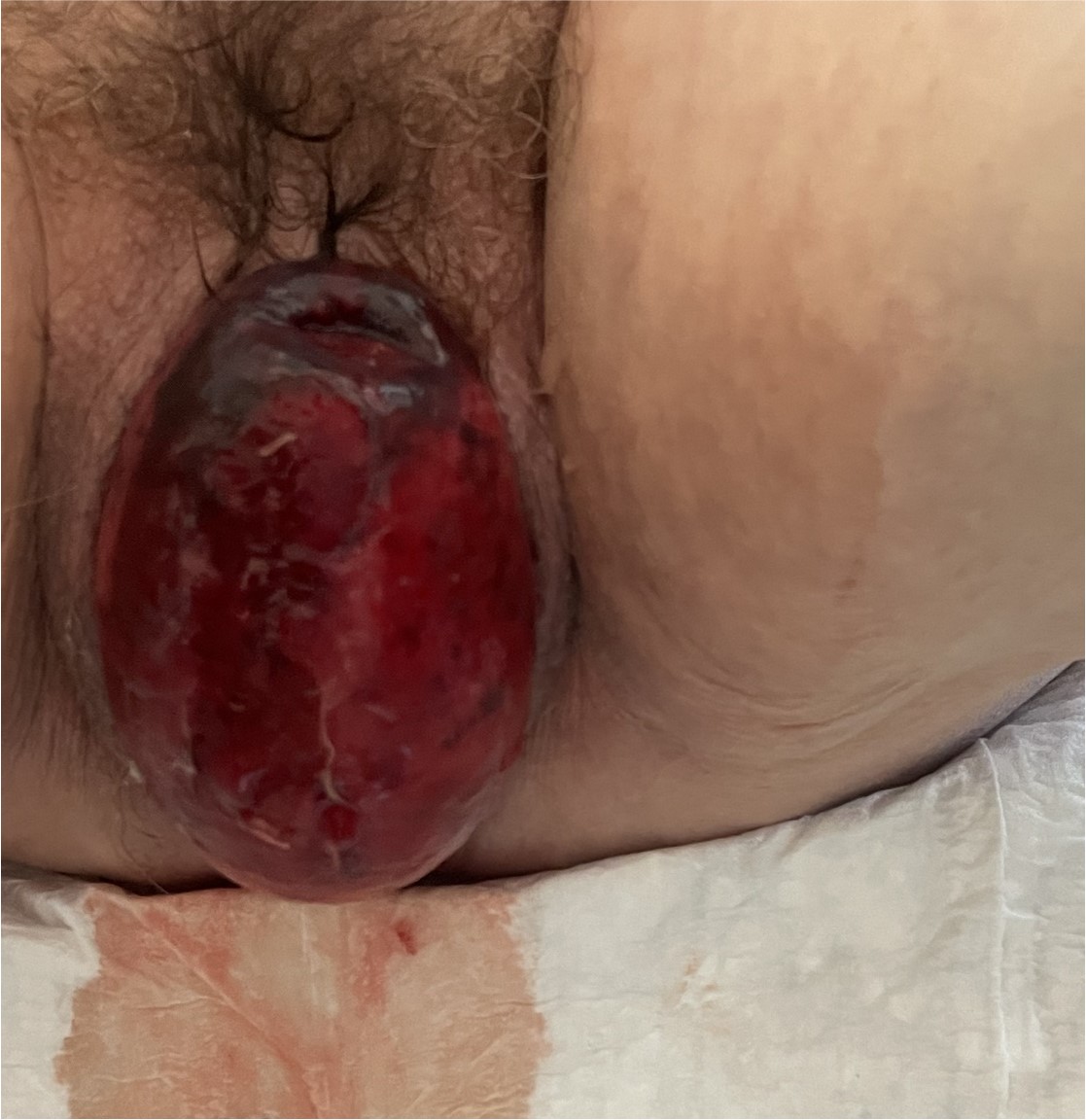
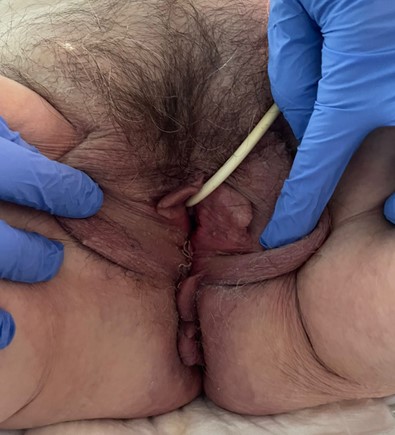
One month later, the patient came to the emergency department with a sensation of a lump in the genitals and scant bleeding. Examination revealed new pessary expulsion with grade IV [9] middle and posterior compartment prolapse, total vaginal eversion and grade IV [9] enterocele, with palpation of intestinal loops through the pessary. The enterocele and uterine cervix looked ulcerated, with bleeding and a purplish color with signs of necrosis (Figures 2 and 3). After bladder catheterization, an unsuccessful attempt was made to reduce the prolapse. Given the risk of incarceration of the bowel loops, it was decided to admit the patient for an urgent surgery.
Figure 2. Grade IV enterocele with grade IV uterine prolapse [9] and vaginal eversion with signs of necrosis.
Figure 3. Grade IV enterocele with grade IV uterine prolapse [9] and vaginal eversion with signs of necrosis.
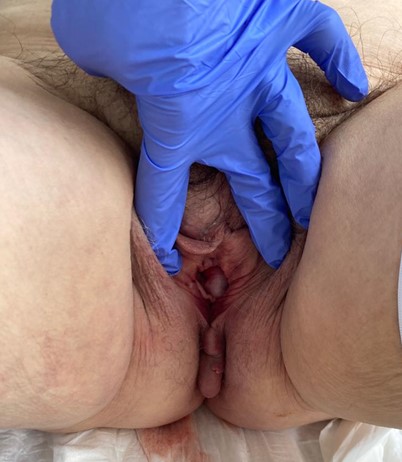
In the first hours of admission, the prolapse is reduced on the hospital ward by placing the patient in the Trendelenburg position and applying local ice (Figure 4).
Figure 4. Reduced prolapse in Trendelenburg position after applying ice in the perineum.
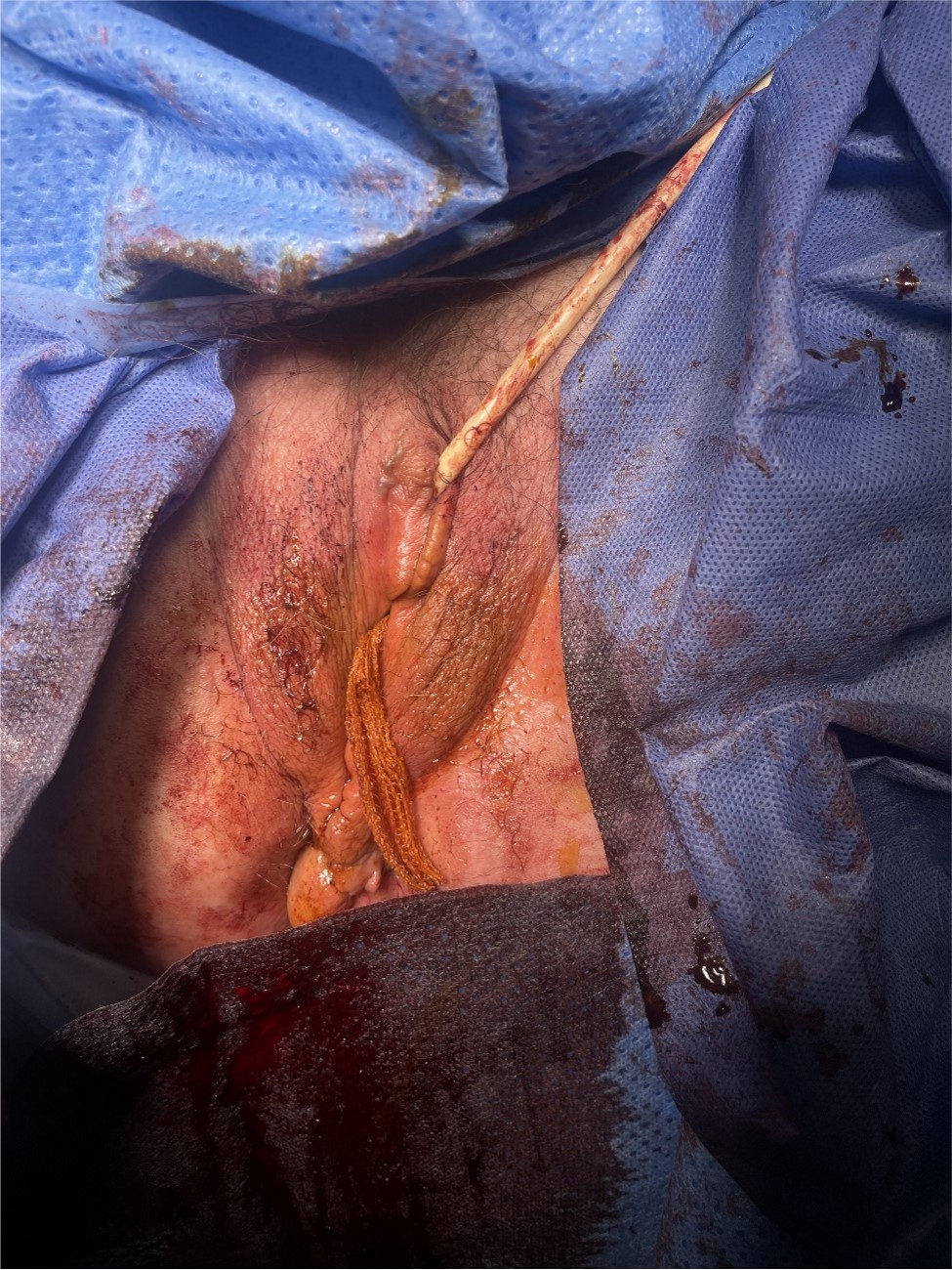
Subsequently, after anticoagulation and atrial fibrillation control by the Cardiology service, urgent surgery was performed with a total vaginal hysterectomy, anterior colporrhaphy, Ritcher's operation, and colpoperineorrhaphy (Figures 5 and 6). The surgery went without incident. During the immediate postoperative period, the patient required permanent bladder catheterization due to elevated post-void residues and was discharged on the fourth day with a bladder catheter, which was successfully removed on the ninth day after surgery.
Figure 5. Immediate surgical outcome with vaginal tamponade and bladder catheterization.
Figure 6. Results in the first 24 hours after surgery.
Discussion
Risk factors for pelvic organ prolapse include obesity, multiparity, menopause, and advanced age [7], all of which are included in the clinical case presented. POP or enterocele can occur with or without a history of hysterectomy, and treatment should be offered to symptomatic patients. Whether conservative or surgical management is chosen, the goal of management is to reduce the prolapse to improve the patient's quality of life [2]. The incidence of enterocele ranges from 0.1% to 16% in women who have undergone previous gynecological surgery [12], however, this is not the case in our patient. Small bowel obstruction as a complication of an enterocele is very rare. Although it may manifest as incomplete emptying of the rectum, the only symptom significantly associated with enterocele is vaginal prolapse itself [2].
In terms of surgical management, there is no single solution for all patients. The kind of surgery depends on different factors such as age, associated comorbidity, sexual activity, type of prolapse etc. [3]. The surgical prognosis will depend on the severity of symptoms, the extent of prolapse, the surgeon's experience and the patient's expectations [7]. It is estimated that surgery is associated with a recurrence rate of around 30% [3,7], so it is very important to select patients carefully and individualize the kind of surgery, reparative or obliterative, associating recurrence prevention techniques when necessary (McCall's culdoplasty and/or fixation of structures to the sacrospinous ligament or Ritcher's operation).
Our case describes an 81-year-old patient, with POP risk factors and severe comorbidities, who initially opted for conservative treatment with a pessary and stitches in the perineum, according to the technique described and published by Pérez et al. in 2023 [10]. After expulsion of the pessary, surgery was considered, but was temporarily postponed due to high anesthetic risk and cardiological problems. During the waiting period, the prolapse progressed and the tissues acquired a purplish and eroded appearance, possibly due to venous stasis, with the risk of vaginal necrosis and intestinal incarceration. At this point, the anesthetic risk is assumed due to the risk of intestinal necrosis and even vaginal rupture and evisceration, and surgical repair is carried out urgently.
It should be noted that prolapse reduction was possible thanks to preoperative management with the patient being placed in the Trendelenburg position together with the application of local ice to the perineum. In this way the tissues were in a better condition to be repaired.
Due to the total eversion of the vagina, in addition to hysterectomy, anterior colporrhaphy and closure of the peritoneal hernia, fixation of the vaginal vault to the right sacrospinous ligament was performed, in order to reduce the risk of subsequent recurrence.
Conclusions
The diagnosis of advanced enterocele with risk of bowel obstruction or even ischemia is a very rare but potentially serious event due to the risk of bowel necrosis, systemic infection or evisceration after vaginal rupture. Its immediate recognition and management are very important for patients with this clinical presentation. Ideally, it would be desirable to first reduce the congested structures in order to manage the tissues in the best possible conditions.
Statements and Declarations
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Authors’ contribution
All authors contributed to the study manuscript and design. Material preparation and data collection were performed by María Cuaresma González, Sonia de Miguel Manso, Paula Suárez Mansilla, and Marta Ibáñez Nieto. The first draft of the manuscript was written by María Cuaresma González. All authors read and approved the final manuscript.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
The authors affirm that human research participants provided informed consent for publication of the image 1, 2, 3, 4, 5, and 6.
References
2. Rafailidis S, Ballas K, Dinas K. Small bowel incarceration associated with posthysterectomy enterocele. International Urogynecology Journal. 2010 May;21:603-5.
3. Giraudet G, Lucot J-P, Quintón J-F, Cosson M. Ginecología – Obstetricia. Tratados EMC. 2017;53(1):1-18.
4. Holley RL. Enterocele: a review. Obstetrical & Gynecological Survey. 1994 Apr;49(4):284-93.
5. Wilkinson KH, Thomas A, Theobald J. Pelvic organ prolapse: an unusual cause of small bowel obstruction. The American Journal of Emergency Medicine. 2019 Sep 1;37(9):1809.e5-1809.e6.
6. Carley ME, Bosquet JG, Stanhope CR. Small bowel obstruction associated with post-hysterectomy vaginal vault prolapse. Obstetrics & Gynecology. 2003 Sep 1;102(3):524-6.
7. Rogers R, Fashokun T. Pelvic organ prolapse in females: Epidemiology, risk factors, clinical manifestations, and management. In: Brubaker L , Eckler K. (Ed). UpToDate. 2023.
8. Milani R, Manodoro S, Cola A, Palmieri S, Reato C, Frigerio M. Transvaginal native-tissue repair of enterocele. International Urogynecology Journal. 2018 Nov;29:1705-7.
9. Sociedad Española de Ginecología y Obstetricia. Prolapso de los órganos pélvicos. Prog Obstet Ginecol 2020;63(1):54-59
10. Pérez-Febles M, De-Miguel-Manso S, García-García E, López-País M, Cuaresma-González M, Ibañez-Nieto M. Pessary with perineal suture for treatment of pelvic organ prolapse: description and benefit of the tech-nique. Archives of Gynecology and Obstetrics. 2023 Mar;307(3):789-95.
11. Yevenes S, Epulef V, Rocco C, Geisse F, Vial M. Local examples of the American Society of anesthesiologists classification. Revista Chilena de Anestesia. 2022;51(3):251-260.
12. Ranney B. Enterocele, vaginal prolapse, pelvic hernia: recognition and treatment. American Journal of Obstetrics and Gynecology. 1981 May 1;140(1):53-61.