Abstract
Introduction: Autonomic dysreflexia is a serious and potentially life-threatening complication of spinal cord injury occurring at T6 or above. It is most often triggered by a sublesional irritative stimulus, typically involving the urinary or gastrointestinal tract.
Although common causes are well recognized, less typical etiologies may complicate the clinical picture.
The hallmark features are arterial hypertension and bradycardia, while associated symptoms may include headache, visual disturbances, dyspnea, nausea, palpitations, nasal congestion, chills, diaphoresis, and flushing.
Case presentation: We report the case of a 46-year-old woman with incomplete tetraplegia at C7, who presented with signs and symptoms of autonomic dysreflexia without an obvious precipitating factor.
Clinical work-up and management of autonomic dysreflexia were initiated.
Results: Imaging studies revealed osteitis of the pubic symphysis associated with a peri-symphysis abscess and bone lysis, following the appearance of a palpable suprapubic mass.
Discussion: Routine follow-up in patients with spinal cord injury includes urodynamic studies, cystoscopy, and ultrasound. In this patient, no conventional risk factors for symphyseal infection were identified, apart from routine urological surveillance procedures.
The etiology of dysreflexia was therefore unusual and its identification unexpected. Antibiotic therapy reduced the episodes of dysreflexia but did not prevent progression of the underlying bone lysis secondary to pubic symphysitis.
A comprehensive etiological assessment is essential in cases of autonomic dysreflexia. Given its potential to endanger life, this condition should always be promptly recognized and appropriately managed.
Keywords
Autonomic dysreflexia, Osteitis pubis, Pubic symphysis, Spinal cord injuries, Tetraplegia, Spinal cord
Introduction
The most frequently reported cardiovascular complications in patients with spinal cord injury are autonomic dysreflexia (AD) and orthostatic hypotension.
Autonomic dysreflexia is a serious complication affecting patients with spinal cord injury at or above the T6 level. The condition is generally triggered by an irritative sublesional stimulus, most commonly involving the urinary and digestive systems, but there are also more complex causes of autonomic dysreflexia, as shown in Table 1 [1].
|
System |
Stimulus |
|
Urinary |
Infection, distension, instrumentation, calculus |
|
Gastrointestinal |
Infection, inflammation, distension, gastric ulcer |
|
Anorectal |
Distension, instrumentation, hemorrhoids, anal fissure |
|
Dermatological |
Infection, ingrown toenail, ulcer pressure |
|
Musculoskeletal |
Fracture, dislocation, heterotopic ossification |
|
Reproductive |
Pregnancy and childbirth, menstruation, adnexal torsion, ejaculation, sexual intercourse |
|
Hematological |
Venous thrombosis, pulmonary embolism |
Autonomic dysreflexia is defined as an increase of 20 mmHg in blood pressure (BP) compared to the patient's usual baseline. Following spinal cord injury, these patients usually have a mean arterial pressure (MAP) that is 15 to 20 mmHg lower than the MBP of the general population.
The main signs of dysreflexia are high blood pressure and bradycardia. The main symptoms are headache, blurred vision, dyspnea, nausea, palpitations, nasal congestion, chills, sweating and flushing [1,2].
Clinical Case
Our patient, a 46-year-old woman, initially sustained a C7 fracture following a road traffic accident in 2002, resulting in incomplete tetraplegia classified as C7 AIS C according to the ISNCSCI classification. The fracture was treated with arthrodesis from C6 to T1. The patient's medical history included several urinary tract infections with indwelling catheters, several surgically treated pressure sores, and resection of colonic polyps.
She presented to the emergency department the week before the consultation with a two-week history of abdominal pain and increased spasticity.
She also reported chills and night sweats. An abdominal CT scan was performed. No abnormalities were noted in the report, and the patient was discharged with a five-day course of amoxicillin–clavulanate. She then presented for a physical medicine consultation two weeks later with persistent symptoms and was hospitalized in our center.
The patient’s usual vital signs were blood pressure 110/80 mmHg and heart rate 80 bpm.
During her hospitalization, she experienced several episodes of autonomic dysreflexia. Although continuous blood pressure monitoring was not available, repeated measurements confirmed a rise up to 160/90 mmHg and her heart rate dropped to 53 bpm, particularly during abdominal palpation and transfers. She complained of headache and abdominal pain, and flushing and sweating were observed during the episodes. Initial non-pharmacological measures (sitting the patient upright, loosening tight clothing, and assessing/managing urinary and fecal triggers) did not result in significant improvement. However, a significant decrease in blood pressure was observed after administration of a short-acting nitrate.
Clinical Examination
Abdominal examination revealed a mass in the suprapubic region, which correlated with the location of the pain. Palpation of this abdominal mass caused discomfort, flushing and sweating in the patient. Blood pressure was measured at 160/90 mmHg.
She was admitted to our department to assess the suprapubic mass and investigate autonomic dysreflexia.
Upon admission, the patient continued to complain of abdominal pain and night sweats. Her vital signs showed a pyrexia of 38.3°C. She also presented with leukorrhea. Blood tests, urine tests and blood cultures were taken. An MRI scan of the pelvis and a bone scan were then requested.
Diagnosis
Blood tests revealed significant inflammation, blood cultures were negative, urinary bacteria corresponded to chronic colonization.
Review of the abdominal CT scan performed in the emergency department revealed a lytic process at the pubic symphysis and symphyseal separation.
The MRI scan showed a parasymphyseal collection associated with pubic osteitis and bone lysis (Figure 1). The collection was aspirated and the fluid analyzed. Cultures obtained from the parasymphyseal collection grew Bacteroides fragilis (4+) and Peptostreptococcus anaerobius under anaerobic conditions.
B. fragilis was susceptible to amoxicillin–clavulanate, piperacillin–tazobactam, imipenem, and metronidazole, and resistant to gentamicin and clindamycin.
A gynecological examination for leukorrhea showed no abnormalities, and an endovaginal ultrasound revealed no fistula. Smears were nevertheless sent for bacteriological analysis. No risky sexual behavior was reported.
Based on MRI findings, positive cultures, and systemic inflammatory markers, we concluded that autonomic dysreflexia was triggered by septic symphysitis with adjacent osteomyelitis, associated with a parasymphyseal collection and bone lysis.
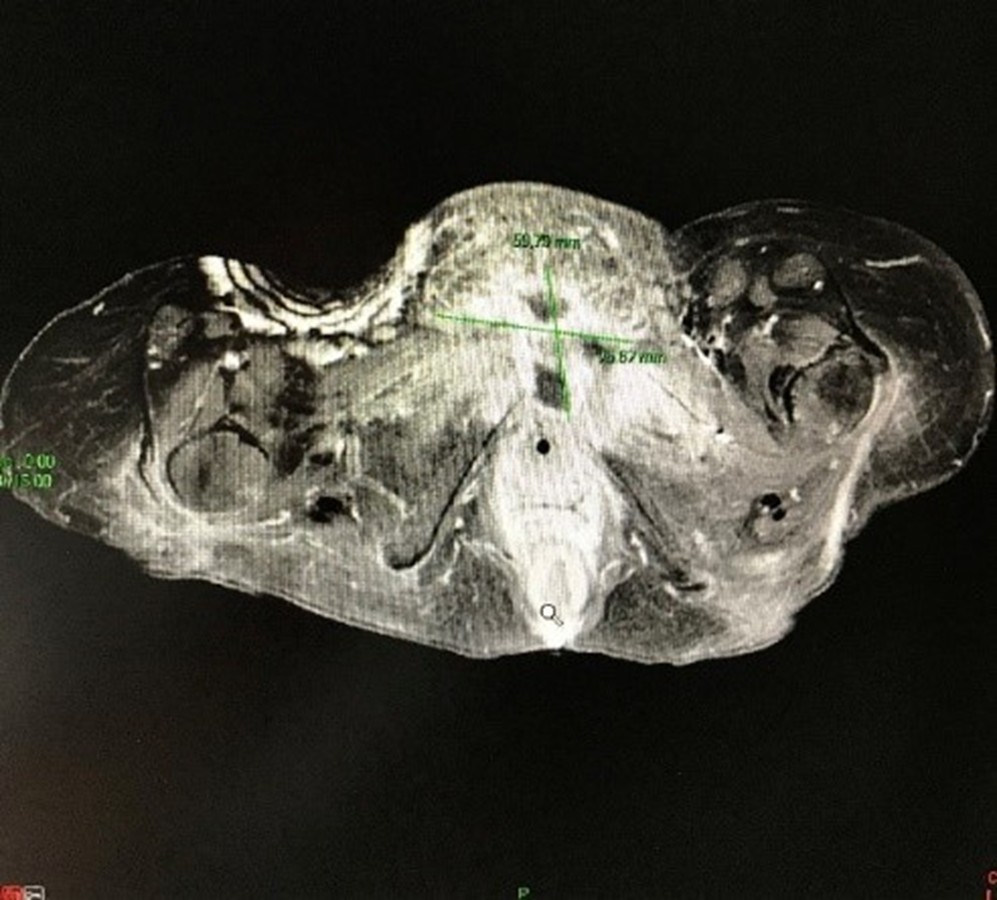
Figure 1. MRI scan shows the presence of a parasymphyseal collection surrounding pubic osteitis with bone lysis.
Treatment
Following the collection of samples by puncture, empirical antibiotic therapy with ceftriaxone (2 g/day) and oral metronidazole for five days, was initiated. Fever resolved within 48 hours, and inflammatory markers progressively decreased. Antibiotic therapy was subsequently switched to oral moxifloxacin to complete a total treatment duration of six weeks.
After antibiotic treatment, she did not experience any further episodes of autonomic dysreflexia or fever and no recurrence at six months. She was able to return home and then moved to Spain.
In patients with spinal cord injury, pubic symphysis infection may result from hematogenous spread, urinary tract colonization, repeated urological instrumentation, or microtrauma related to altered biomechanics and sensory impairment. In the present case, no recent pelvic surgery or trauma was identified. Chronic urinary incontinence and long-standing neurogenic bladder dysfunction were considered the most plausible predisposing factors, although a definitive portal of entry could not be established.
Discussion
The assessment and monitoring of the neurological bladder in patients with spinal cord injury includes an annual urodynamic assessment, an ultrasound scan to study the impact on the upper urinary tract, and an annual cystoscopy after 10 years of self-catheterization to rule out any suspicious lesions [3]. These assessments may themselves trigger AD [4]. The same applies to the evaluation of certain digestive problems, which may include constipation, incontinence, intestinal hemorrhages or hemorrhoids. Some of these conditions must be evaluated by colonoscopy, which may also trigger AD.
Our patient had no other risk factors for symphysis infection other than her spinal cord injury, urinary incontinence, and the need for follow-up urological examinations.
This cause of dysreflexia is uncommon and its discovery was unexpected. Antibiotic treatment reduced dysreflexia but did not resolve the bone lysis resulting from the symphysis.
There are many causes of autonomic dysreflexia, but they are not always obvious. The presence of the mass in the suprapubic region guided investigations. Without this clinical finding, investigations would likely have been less targeted, potentially leading to delayed diagnosis and treatment.
Conclusion
Autonomic dysreflexia is hardly known among the general population and the medical community. As a result, treatment may be delayed during an acute episode of AD, which can lead to fatal complications. Medical staff and patients' families and friends need to be made aware of this type of complication of spinal cord injury.
The assessment of dysreflexia must be exhaustive and lead to the final etiology. Dysreflexia can be life-threatening and must not be overlooked.
References
2. Eldahan KC, Rabchevsky AG. Autonomic dysreflexia after spinal cord injury: Systemic pathophysiology and methods of management. Auton Neurosci. 2018 Jan;209:59–70.
3. Even-Schneider A, Denys P, Chartier-Kastler E, Ruffion A. Troubles vésico-sphinctériens et traumatismes médullaires [Lower urinary tract dysfunction and spinal cord injury]. Prog Urol. 2007 May;17(3):347–51.
4. Shergill IS, Arya M, Hamid R, Khastgir J, Patel HR, Shah PJ. The importance of autonomic dysreflexia to the urologist. BJU Int. 2004 May;93(7):923–6.
